Presentation of Characteristics and Origin of Immune Cells Causing Lung Damage After COVID-19 Infection
The research group led by Su-Hyung Park, the director of Center for Epidemic Preparedness, conducted a joint study with the College of Medicine at Chungbuk National University and obtained meaning accomplishments in relation to the lung pathology of COVID-19. They analyzed the qualitative and quantitative changes of the immune responses from the peak of the COVID-19 virus growth to the recovery period to investigate the characteristics and origin of the specific immune cells that cause pulmonary damage. Director Park said that the biggest gain from the study was that the time-dependent variation immediately after the COVID-19 infection was precisely investigated in comparison with the time before the infection.
|Help for Establishing Treatment Strategy for Serious COVID-19 Patients|
Understanding of macrophage in COVID-19
“The scientific and medical significance of our results is that we identified a specific inflammatory macrophage as the cause of the post-infection lung damage, providing the basis for preparing precise immunosuppressive treatment strategy that is applied to serious COVID-19 patients. Currently, steroids are often used to a therapy for serious COVID-19 patients, and various candidates are under the clinical studies. Our study presented a specific macrophage group that causes the hyper-inflammatory responses, as a target for controlling the lung damage in the COVID-19 patients. We expect that our results can help to develop a therapy for serious COVID-19 patients.”
Macrophages are immune cells that recognize virus-infected cells or cancer cells to directly remove them through phagocytosis. They are like ‘rapid-reaction forces’ of our body that remove virus-infected cells in the lung tissues after the initial stage of the COVID-19 infection. However, the hyper-activation of the macrophages causes the excessive secretion of inflammatory cytokines, resulting in a lung damage and the severity of the patient conditions.
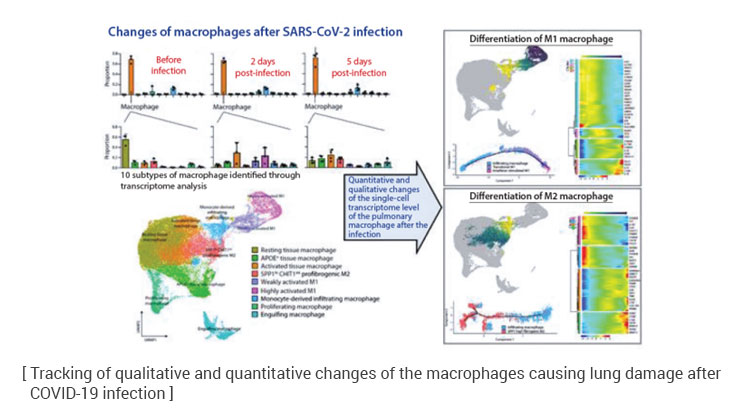
Director Park’s group performed a precise analysis of the changes in the pulmonary immune cells by single-cell RNA sequencing when the infection was progressing in ferrets, which were a COVID-19 infected animal model. They found that the macrophages, which accounts for most of the pulmonary immune cells, may be classified into 10 subtypes. Some of the subtypes, showing the characteristics of inflammatory macrophages strongly, contribute to the removal of the viruses, and at the same time, play the key role in causing the damage in some tissues. The functioning of these subtypes showed a high similarity to the changes observed in the lung tissues of the serious COVID-19 patients. Therefore, the research group was able to present the mechanism of the shifting to serious COVID-19 patients and the immune cells that cause it.
Single-cell RNA sequencing as a technology drawing much attention
Single-cell RNA sequencing, the method employed in their study, is also drawing much attention. This technology enables the researchers to measure the expression level of thousands of genes from a single cell. Hence, it is regarded as a technology that has drastically broaden the visual field of biology. Director Park said that single-cell RNA sequencing can be used for not only the simultaneous analysis of heterogeneous cells that are present in a tissue or multiple tissues but also the comparison of the heterogeneity among the cells, increasing the physiological understanding. He commented, “Furthermore, the technology helps to understand the disease onset mechanisms by comparatively analyzing the gene expression levels between normal and pathological somatic cells.”
Prof.Su-Hyung Park
2021 Annual Report
